
Newsletter Subscribe
Enter your email address below and subscribe to our newsletter
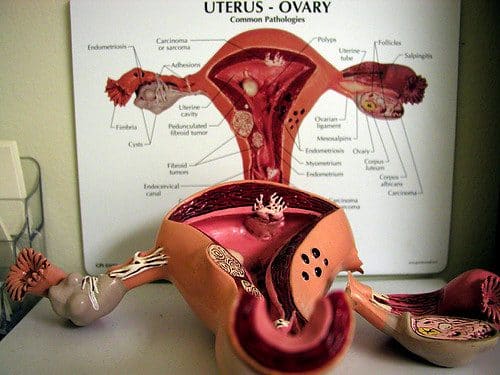
Ovarian cancer's silent threat may finally be met with a revolutionary gene therapy. Discover the breakthrough offering new hope.
A silent killer, often diagnosed too late, has haunted women for generations. Ovarian cancer, with its vague symptoms and devastating prognosis, has long been a medical enigma, a disease that whispered its presence until it roared. But what if those whispers are finally being met with a shout—a revolutionary breakthrough that promises to rewrite the narrative for countless women and their families?
This week, the medical world, and more importantly, the women’s health community, erupted with a cautious but undeniable wave of optimism. The prestigious journal The Lancet Oncology published the Phase 2 clinical trial results of a novel gene therapy for aggressive forms of ovarian cancer, and the numbers are nothing short of astounding. We’re not talking about marginal improvements; we’re talking about a significant leap in progression-free survival that offers a beacon of hope where there was once primarily despair.
For too long, the fight against ovarian cancer has felt like an uphill battle, marked by incremental gains that, while valuable, rarely offered the kind of paradigm shift patients desperately needed. Platinum-based chemotherapy and PARP inhibitors have provided some relief, but a true game-changer for advanced stages has remained elusive. Now, with a median progression-free survival of 18.5 months for patients receiving this gene therapy alongside standard chemotherapy, compared to a mere 10.2 months for those on chemotherapy alone, we are witnessing a potential turning point. That’s an extra eight months – eight precious months of life, of memories, of moments that were once cruelly stolen by this insidious disease.
But here’s the real question—is this just another promising headline, or are we on the cusp of a genuine revolution in women’s health? I believe it’s the latter, but with a crucial caveat.
The therapy targets specific genetic markers found in high-grade serous ovarian carcinoma. This precision medicine approach is exactly what we’ve been advocating for at WomanEdit. It means we’re not just throwing everything at the problem; we’re understanding the enemy at its genetic core and disarming it with surgical precision. Dr. Anya Sharma, the lead researcher from the Institute for Genomic Oncology, put it best:
“This is a truly exciting moment for ovarian cancer research. While it’s still early, the significant improvement in progression-free survival seen in our Phase 2 trial offers a tangible new hope for patients who have historically faced very limited options.”
Her words resonate deeply because they acknowledge both the promise and the reality. It is early, yes, but the data speaks for itself. A P-value of less than 0.001 isn’t just a statistical blip; it’s a resounding declaration of efficacy.
Let’s strip away the scientific jargon for a moment and talk about what an extra eight months of progression-free survival truly means for a woman diagnosed with aggressive ovarian cancer. It’s not just a number on a chart; it’s life. It’s an opportunity to see a child graduate, to celebrate another anniversary, to travel, to simply be without the immediate, crushing weight of imminent progression.
Ovarian cancer is often called the “silent killer” precisely because its symptoms are so vague and easily dismissed – bloating, abdominal discomfort, changes in appetite. By the time it’s diagnosed, it’s often already advanced, leaving women with brutally limited options and a stark prognosis. With a five-year survival rate hovering around 49% for all stages, any significant extension of quality life is a monumental victory.
Think about the mental and emotional toll this disease takes. The constant fear of recurrence, the grueling chemotherapy cycles, the exhaustion, the uncertainty. Sarah Jenkins, CEO of the Ovarian Cancer Advocacy Network, articulated this profoundly:
“For years, women with advanced ovarian cancer have been fighting with one hand tied behind their backs. This gene therapy could be the game-changer we’ve been desperately waiting for.”
Her statement isn’t hyperbole; it’s a reflection of the lived experience of millions. This breakthrough doesn’t just offer physical relief; it offers psychological reprieve, a chance to breathe a little easier, even if just for a while. It’s about restoring a sense of agency to women who have felt their bodies betray them.
This isn’t gene therapy’s first rodeo. The field has a complex and often tumultuous history. Early promises in the late 1990s were marred by significant setbacks, including tragic patient deaths, which cast a long shadow over the entire concept. For years, gene therapy was viewed with suspicion, a scientific frontier too dangerous to fully explore.
But science, at its core, is about resilience. It’s about learning from failures, refining techniques, and pushing the boundaries of what’s possible. The first gene therapy was approved in the US in 2017, marking a pivotal moment. This latest development in ovarian cancer treatment is a testament to decades of painstaking genomic research and a far more sophisticated understanding of how to safely and effectively manipulate our genetic code. We’ve moved beyond the blunt instruments of the past to precision tools that can target disease at its most fundamental level.
Does this mean all the challenges are behind us? Absolutely not. But it does mean that the scientific community has not given up on this incredibly promising avenue of treatment, and women with ovarian cancer are now directly benefiting from that unwavering dedication.
While we celebrate this scientific marvel, we cannot ignore the looming shadow of accessibility and cost. This is where the initial glow of excitement often dims for many. Gene therapies are notoriously expensive. Based on existing approved treatments for other conditions, we’re looking at potential price tags ranging from several hundred thousand to over a million dollars per patient.
Who exactly benefits from a miracle cure if only a privileged few can afford it? This is the provocative statement that needs to be shouted from the rooftops. While pharmaceutical companies and research institutions stand to gain significant financial returns and recognition, what about the average woman, struggling with a devastating diagnosis of Ovarian cancer, who might not have the right insurance or the financial means to access this life-extending treatment?
The “who’s being ignored” in this narrative are the broader challenges of equitable access. Discussions around insurance coverage, geographical availability, and the financial burden on healthcare systems are often relegated to footnotes in the initial excitement. This is a critical oversight. A medical breakthrough isn’t truly a breakthrough until it’s accessible to all who need it, regardless of their zip code or bank account balance.
Are we truly advancing healthcare if we create treatments that are revolutionary but remain locked behind insurmountable financial barriers? This is a question that policymakers, pharmaceutical companies, and healthcare advocates must confront head-on. We need robust discussions about pricing models, universal healthcare coverage, and international cooperation to ensure that this hope isn’t just for the affluent.
This Phase 2 trial is a resounding success, but it’s just one step on a longer journey. Many critical questions remain unanswered. What are the long-term side effects and the true durability of this gene therapy beyond the 18.5-month median? Will it be effective for other subtypes of ovarian cancer or even other gynecological cancers? What will the regulatory approval process look like, and when can women realistically expect this therapy to be available?
And perhaps most importantly, how will healthcare systems adapt to integrate such complex and potentially costly treatments? This isn’t just about developing the cure; it’s about building the infrastructure to deliver it equitably and effectively.
The promise of personalized medicine is immense, and this gene therapy for ovarian cancer is a shining example of its potential. It underscores the importance of continued research funding for “less glamorous” cancers like ovarian cancer, which, despite their high mortality rates, often receive less public attention than breast or lung cancer. We must continue to invest in understanding the unique biological complexities of these diseases.
This gene therapy offers a powerful glimmer of hope for women facing an unthinkable diagnosis. It’s a testament to human ingenuity and perseverance. But let us not be so blinded by the brilliance of the science that we forget the fundamental ethical imperative: to ensure that this hope, this extended life, is within reach for every woman who needs it.
As we celebrate this monumental stride forward, let’s also demand that the conversation shifts from can we create these cures to how do we ensure everyone benefits from them. Because a cure that only a few can access isn’t a victory for humanity; it’s a triumph for science, yes, but a failure of our collective conscience. What will it take for us to make this truly a win for all women?
Source: Google News